Stevens-Johnson Syndrome: The Life-Threatening Drug Reactions
- Pharm. Onyehalu Jennifer

- Mar 27
- 3 min read
Imagine taking a medication to feel better only for your body to react in a way that becomes life-threatening.
This is the reality of Stevens-Johnson Syndrome (SJS); a rare but severe condition that affects the skin and mucous membranes.
What Is Stevens-Johnson Syndrome?
Stevens-Johnson Syndrome is a serious hypersensitivity reaction, most often triggered by medications.
It usually starts with flu-like symptoms but quickly progresses into a dangerous skin condition where the top layer of the skin begins to die and peel away.
Stevens-Johnson syndrome (SJS) and its more severe counterpart, Toxic Epidermal Necrolysis (TEN), are rare but potentially fatal immune-mediated reactions that primarily target the skin and mucous membranes. Often described as "the skin melting off," SJS is a medical emergency that requires immediate hospitalization and a specialized multidisciplinary approach.

The SJS-TEN Spectrum
Medical professionals view SJS and TEN as a single disease spectrum distinguished by the extent of skin detachment:
SJS: Affects less than 10% of the total body surface area (BSA).
SJS/TEN Overlap: Involves 10% to 30% of the body surface.
Toxic Epidermal Necrolysis (TEN): The most severe form, involving more than 30% of the body surface.
The mortality rate increases significantly with the severity of the reaction, ranging from approximately <10% for SJS to over 30% for TEN.
Common Triggers and Risk Factors
In more than 80% of cases, SJS is triggered by an adverse reaction to a medication. While almost any drug can be the culprit, certain classes are high-risk:
Antibiotics: Sulfonamides (e.g., Bactrim), penicillins, and cephalosporins.
Antiepileptics: Carbamazepine, phenytoin, lamotrigine, and phenobarbital.
Sulfonamides: cotrimoxazole, sulfasalazine
Allopurinol: A common medication used to treat gout.
Pain Relievers: Nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen or naproxen and acetaminophen.
Non-Drug Causes: Infections, particularly Mycoplasma pneumoniae (the most common cause in children) and Herpes simplex virus, can also trigger the syndrome.
Genetic Predisposition: Specific genetic markers significantly increase the risk for certain populations. For instance, the HLA-B*1502 allele is strongly linked to carbamazepine-induced SJS in individuals of Han Chinese and other Southeast Asian ancestries.

Clinical Presentation: From Flu to Full-Body Rash
The onset of SJS is typically sudden and progresses through distinct phases:
The Prodrome: 1 to 3 days before the rash appears, patients often experience flu-like symptoms, including fever, sore throat, cough, and burning eyes.
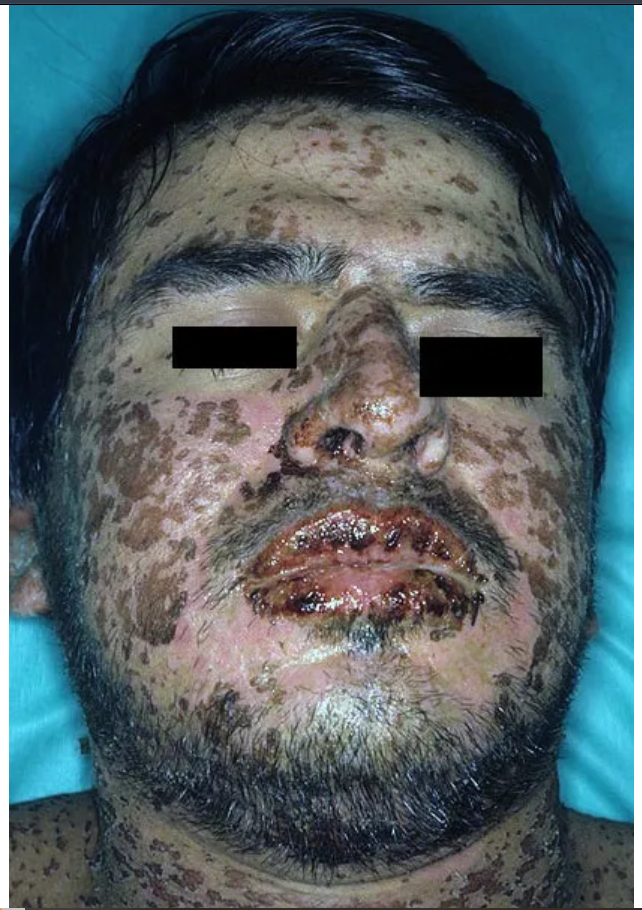
The Rash: A painful, flat red or purple rash begins, often on the face and trunk, before spreading.
Blistering & Peeling: Blisters form and coalesce, leading to sheet-like peeling of the skin. A hallmark sign is the Nikolsky sign, where gentle pressure causes the top layer of skin to slide off.
Mucosal Involvement: Nearly all patients suffer from painful sores in the mouth, eyes, and genital regions, which can make eating, urinating, or even opening the eyes impossible.
Why Is It Dangerous?
Stevens-Johnson Syndrome is a medical emergency.
It can lead to:
Severe dehydration
Infections
Organ damage
Vision problems
Death (in severe cases)
The skin essentially loses its ability to protect the body.
Who Is at Risk?
Some people have a higher risk, including:
Individuals starting new medications
People with weakened immune systems
Those with a history of drug reactions
Certain genetic backgrounds
Emergency Management and Treatment
Survival depends on early diagnosis and rapid intervention:
Cessation of the Trigger: The most critical step is the immediate withdrawal of the suspected causative medication.
Specialized Care: Patients are ideally treated in a burn unit or intensive care unit (ICU) for sterile wound management and intensive fluid/electrolyte replacement.
Systemic Therapies: While controversial, doctors may use high-dose corticosteroids, intravenous immunoglobulin (IVIg), or cyclosporine to dampen the immune response.
Emerging Treatments: Recent research highlights the potential of TNF-alpha inhibitors (like etanercept) and JAK inhibitors to speed up skin healing.
Others include pain medications and infection prevention.
The Long Road to Recovery
For survivors, the acute phase is only the beginning. Long-term "sequelae" (after-effects) are common and can be life-altering:
Vision Loss: Chronic dry eye, scarring, and even blindness can occur if ocular involvement is severe.
Skin & Nail Changes: Permanent scarring, changes in skin color (dyspigmentation), and the loss of fingernails or toenails.
Psychological Toll: Survivors frequently report high rates of PTSD (up to 27%), depression, and an intense "fear of medications."
If you suspect you are experiencing an early reaction to a new medication, seek emergency care immediately at a hospital equipped with a burn unit or dermatology specialist.
Final Thoughts
Stevens-Johnson Syndrome may be rare, but its impact is severe.
The most important thing is awareness.
A simple reaction to a drug should never be ignored, especially when it involves rash, fever, and unusual discomfort.
Knowing the signs could save a life, possibly yours or someone close to you.











Comments